Easy Methods To Care For Fallen Arches
Overview
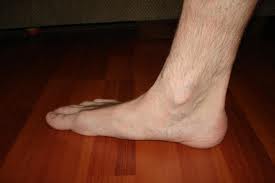
Fallen arches or flat feet is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Flat feet (also called pes planus or fallen arches) is a formal reference to a medical condition in which the arch of the foot collapses, with the entire sole of the foot coming into complete or near-complete contact with the ground. In some individuals (an estimated 20-30% of the general population) the arch simply never develops in one foot (unilaterally) or both feet (bilaterally).
Causes
Inflammatory arthritis, such as rheumatoid arthritis, can cause a painful flatfoot. This type of arthritis attacks not only the cartilage in the joints, but also the ligaments that support the foot. Inflammatory arthritis not only causes pain, but also causes the foot to change shape and become flat. The arthritis can affect the back of the foot or the middle of foot, both of which can result in a fallen arch. An injury to the ligaments in the foot can cause the joints to fall out of alignment. The ligaments support the bones and prevent them from moving. If the ligaments are torn, the foot will become flat and painful. This more commonly occurs in the middle of the foot (Lisfranc injury), but can also occur in the back of the foot. In addition to ligament injuries, fractures and dislocations of the bones in the midfoot can also lead to a flatfoot deformity. People with diabetes or with a nerve problem that limits normal feeling in the feet, can have arch collapse. This type of arch collapse is typically more severe than that seen in patients with normal feeling in their feet. This is because patients do not feel pain as the arch collapses. In addition to the ligaments not holding the bones in place, the bones themselves can sometimes fracture and disintegrate, without the patient feeling any pain. This may result in a severely deformed foot that is very challenging to correct with surgery. Special shoes or braces are the best method for dealing with this problem.
Symptoms
Knee/Hip/Back Pain - When the arch collapses in the foot, it triggers a series of compensations up the joint chain, leading to increased stress on the knee, pelvis and low back. Plantar fasciitis - This condition is characterized by heel pain, especially with the first few steps you take. The plantar fascia stretches as the arch falls, putting stress on the heel. Bunions - If you see a bony bump developing at the base of your big toe, you are likely developing a bunion. It may be swollen, red or painful when it rubs against your shoe. A flattened arch spreads the forefoot and causes the big toe to deviate toward the second toe. Shin splints - This term generally refers to pain anywhere along the shinbone. It is typically due to overuse and is aggravated after exercise and activity.
Diagnosis
Determining whether you have fallen arches may be as easy as looking at the shape of the middle bottom of your foot. Is there any kind of arch there? If you cannot find any kind of arch, you may have a flat foot. There are, however, other ways to decide in case you're still not sure. Another way to figure out if you have flat feet is to look at a few pairs of your shoes. Where do you see the most wear on the heels? If you notice significant wear in the heel and the ball of the foot extending to the big toe, this means you are overpronating. Overpronators roll their feet too far inward and commonly have fallen arches. To figure out if you have flat feet, you can also do an easy test. Get the bottoms of your feet wet and then step on to a piece of paper carefully. Step off the paper and take a look at the print your foot made. If your print looks like the entire bottom of a foot, your feet are flat. People with an arch will be missing part of the foot on their print since the arch is elevated off of the paper. Regular visits to your podiatrist are highly recommended.
fallen arches support
Non Surgical Treatment
The simplest form of treatment is the use of custom fitted orthotics. For this, it is best to see a podiatrist, who is a trained medical professional that assesses feet and gives you a prescription for the orthotic. If the orthotics do not work - or if the deformity is very severe - then surgical management may be needed. There is a very wide range of procedures available, with varying downtimes and complexity. The simplest procedure of all is a simple calf release. This can be done at the back of the knee or the calf, and has a very quick recovery. It is a day-surgery procedure, and the patient can walk immediately after the surgery without the need for a cast. Recovery back to jogging can be as early as three weeks. The calf release stops the deforming force but obviously does not correct the arch itself. It is usually done in combination with some of the other procedures mentioned below. Done by itself, the patient will probably still require orthotics but by releasing the calf, it allows the orthotics to be much more effective. The other end of the spectrum is a complete reconstruction of the arch with bone work and screws to fuse joints.
Surgical Treatment

Fallen arches may occur with deformities of the foot bones. Tarsal coalition is a congenital condition in which the bones of the foot do not separate from one another during development in the womb. A child with tarsal coalition exhibits a rigid flat foot, which can be painful, notes the patient information website eOrthopod. Surgery may prove necessary to separate the bones. Other foot and ankle conditions that cause fallen arches may also require surgery if noninvasive treatments fail to alleviate pain and restore normal function.

Fallen arches or flat feet is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Flat feet (also called pes planus or fallen arches) is a formal reference to a medical condition in which the arch of the foot collapses, with the entire sole of the foot coming into complete or near-complete contact with the ground. In some individuals (an estimated 20-30% of the general population) the arch simply never develops in one foot (unilaterally) or both feet (bilaterally).
Causes
Inflammatory arthritis, such as rheumatoid arthritis, can cause a painful flatfoot. This type of arthritis attacks not only the cartilage in the joints, but also the ligaments that support the foot. Inflammatory arthritis not only causes pain, but also causes the foot to change shape and become flat. The arthritis can affect the back of the foot or the middle of foot, both of which can result in a fallen arch. An injury to the ligaments in the foot can cause the joints to fall out of alignment. The ligaments support the bones and prevent them from moving. If the ligaments are torn, the foot will become flat and painful. This more commonly occurs in the middle of the foot (Lisfranc injury), but can also occur in the back of the foot. In addition to ligament injuries, fractures and dislocations of the bones in the midfoot can also lead to a flatfoot deformity. People with diabetes or with a nerve problem that limits normal feeling in the feet, can have arch collapse. This type of arch collapse is typically more severe than that seen in patients with normal feeling in their feet. This is because patients do not feel pain as the arch collapses. In addition to the ligaments not holding the bones in place, the bones themselves can sometimes fracture and disintegrate, without the patient feeling any pain. This may result in a severely deformed foot that is very challenging to correct with surgery. Special shoes or braces are the best method for dealing with this problem.
Symptoms
Knee/Hip/Back Pain - When the arch collapses in the foot, it triggers a series of compensations up the joint chain, leading to increased stress on the knee, pelvis and low back. Plantar fasciitis - This condition is characterized by heel pain, especially with the first few steps you take. The plantar fascia stretches as the arch falls, putting stress on the heel. Bunions - If you see a bony bump developing at the base of your big toe, you are likely developing a bunion. It may be swollen, red or painful when it rubs against your shoe. A flattened arch spreads the forefoot and causes the big toe to deviate toward the second toe. Shin splints - This term generally refers to pain anywhere along the shinbone. It is typically due to overuse and is aggravated after exercise and activity.
Diagnosis
Determining whether you have fallen arches may be as easy as looking at the shape of the middle bottom of your foot. Is there any kind of arch there? If you cannot find any kind of arch, you may have a flat foot. There are, however, other ways to decide in case you're still not sure. Another way to figure out if you have flat feet is to look at a few pairs of your shoes. Where do you see the most wear on the heels? If you notice significant wear in the heel and the ball of the foot extending to the big toe, this means you are overpronating. Overpronators roll their feet too far inward and commonly have fallen arches. To figure out if you have flat feet, you can also do an easy test. Get the bottoms of your feet wet and then step on to a piece of paper carefully. Step off the paper and take a look at the print your foot made. If your print looks like the entire bottom of a foot, your feet are flat. People with an arch will be missing part of the foot on their print since the arch is elevated off of the paper. Regular visits to your podiatrist are highly recommended.
fallen arches support
Non Surgical Treatment
The simplest form of treatment is the use of custom fitted orthotics. For this, it is best to see a podiatrist, who is a trained medical professional that assesses feet and gives you a prescription for the orthotic. If the orthotics do not work - or if the deformity is very severe - then surgical management may be needed. There is a very wide range of procedures available, with varying downtimes and complexity. The simplest procedure of all is a simple calf release. This can be done at the back of the knee or the calf, and has a very quick recovery. It is a day-surgery procedure, and the patient can walk immediately after the surgery without the need for a cast. Recovery back to jogging can be as early as three weeks. The calf release stops the deforming force but obviously does not correct the arch itself. It is usually done in combination with some of the other procedures mentioned below. Done by itself, the patient will probably still require orthotics but by releasing the calf, it allows the orthotics to be much more effective. The other end of the spectrum is a complete reconstruction of the arch with bone work and screws to fuse joints.
Surgical Treatment

Fallen arches may occur with deformities of the foot bones. Tarsal coalition is a congenital condition in which the bones of the foot do not separate from one another during development in the womb. A child with tarsal coalition exhibits a rigid flat foot, which can be painful, notes the patient information website eOrthopod. Surgery may prove necessary to separate the bones. Other foot and ankle conditions that cause fallen arches may also require surgery if noninvasive treatments fail to alleviate pain and restore normal function.
All You Need To Know About Heel Painfulness
Overview

The heel bone is the largest of the 26 bones in the human foot, which also has 33 joints and a network of more than 100 tendons, muscles, and ligaments. Like all bones, it is subject to outside influences that can affect its integrity and its ability to keep us on our feet. Heel pain, sometimes disabling, can occur in the front, back, or bottom of the heel.
Causes
Plantar fasciitis is caused by inflammation and irritation of the tight tissue forming the arch of the foot. The most common cause of heel pain, it typically affects men, aged 40 - 70 who are physically active. The bottom or inside of the foot and / or heel (where heel and arch meet) may hurt or cause severe pain upon standing after resting -- or most often, when arising in the morning. The pain is usually experienced within the first few steps and is often characterized as "walking on nails" or knife blades. The pain may let up after walking a bit but most commonly returns after prolonged movement or a rest.
Symptoms
Initially, this pain may only be present when first standing up after sleeping or sitting. As you walk around, the muscle and tendon loosen and the pain goes away. As this problem progresses, the pain can be present with all standing and walking. You may notice a knot or bump on the back of the heel. Swelling may develop. In some cases, pressure from the back of the shoe causes pain.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
When consulting a doctor about heel pain, a patient can expect to be questioned about their level of pain, how long they?ve been experiencing it, and which activities aggravate or alleviate the condition. The doctor may order x-rays, a physical therapy regimen, or refer the afflicted individual to an orthopedic specialist for further examination. The doctor may attempt to recreate conditions that cause the heel pain to flare up in order to study reaction and cause in the patient, but this will be temporary and the doctor will stop this test at the request of the patient. A patient with heel pain may also be fitted with special inserts for their shoes to help correct arch and heel problems that cause pain. Heel problems can range from the mildly irritating to the nearly devastating, but proper prevention in care will help keep each step pain free. Advanced orthopedics, pain management, and technologically-honed surgical techniques ensure that no patient needs to suffer with the discomfort of heel pain and the restrictions it imposes on an active lifestyle.
Surgical Treatment
If treatment hasn't worked and you still have painful symptoms after a year, your GP may refer you to either an orthopaedic surgeon, a surgeon who specialises in surgery that involves bones, muscles and joints or a podiatric surgeon, a podiatrist who specialises in foot surgery. Surgery is sometimes recommended for professional athletes and other sportspeople whose heel pain is adversely affecting their career. Plantar release surgery is the most widely used type of surgery for heel pain. The surgeon will cut the fascia to release it from your heel bone and reduce the tension in your plantar fascia. This should reduce any inflammation and relieve your painful symptoms. Surgery can be performed either as open surgery, where the section of the plantar fascia is released by making a cut into your heel or endoscopic or minimal incision surgery - where a smaller incision is made and special instruments are inserted through the incision to gain access to the plantar fascia. Endoscopic or minimal incision surgery has a quicker recovery time, so you will be able to walk normally much sooner (almost immediately), compared with two to three weeks for open surgery. A disadvantage of endoscopic surgery is that it requires both a specially trained surgical team and specialised equipment, so you may have to wait longer for treatment than if you were to choose open surgery. Endoscopic surgery also carries a higher risk of damaging nearby nerves, which could result in symptoms such as numbness, tingling or some loss of movement in your foot. As with all surgery, plantar release carries the risk of causing complications such as infection, nerve damage and a worsening of your symptoms after surgery (although this is rare). You should discuss the advantages and disadvantages of both techniques with your surgical team.
heel bursitis
Prevention

Heel pain is commonly caused from shoes that do not fit properly. In addition, shoes need to have ample cushioning and support, particularly through the heel, ball of the foot, and arch. Shoes should also be replaced if they become too worn. One sure sign of wear and tear is overly worn areas of a shoe's insoles. If the heel or ball of the foot is particularly worn, damage could easily occur since the bottom of the foot is not getting the cushioning it needs.

The heel bone is the largest of the 26 bones in the human foot, which also has 33 joints and a network of more than 100 tendons, muscles, and ligaments. Like all bones, it is subject to outside influences that can affect its integrity and its ability to keep us on our feet. Heel pain, sometimes disabling, can occur in the front, back, or bottom of the heel.
Causes
Plantar fasciitis is caused by inflammation and irritation of the tight tissue forming the arch of the foot. The most common cause of heel pain, it typically affects men, aged 40 - 70 who are physically active. The bottom or inside of the foot and / or heel (where heel and arch meet) may hurt or cause severe pain upon standing after resting -- or most often, when arising in the morning. The pain is usually experienced within the first few steps and is often characterized as "walking on nails" or knife blades. The pain may let up after walking a bit but most commonly returns after prolonged movement or a rest.
Symptoms
Initially, this pain may only be present when first standing up after sleeping or sitting. As you walk around, the muscle and tendon loosen and the pain goes away. As this problem progresses, the pain can be present with all standing and walking. You may notice a knot or bump on the back of the heel. Swelling may develop. In some cases, pressure from the back of the shoe causes pain.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
When consulting a doctor about heel pain, a patient can expect to be questioned about their level of pain, how long they?ve been experiencing it, and which activities aggravate or alleviate the condition. The doctor may order x-rays, a physical therapy regimen, or refer the afflicted individual to an orthopedic specialist for further examination. The doctor may attempt to recreate conditions that cause the heel pain to flare up in order to study reaction and cause in the patient, but this will be temporary and the doctor will stop this test at the request of the patient. A patient with heel pain may also be fitted with special inserts for their shoes to help correct arch and heel problems that cause pain. Heel problems can range from the mildly irritating to the nearly devastating, but proper prevention in care will help keep each step pain free. Advanced orthopedics, pain management, and technologically-honed surgical techniques ensure that no patient needs to suffer with the discomfort of heel pain and the restrictions it imposes on an active lifestyle.
Surgical Treatment
If treatment hasn't worked and you still have painful symptoms after a year, your GP may refer you to either an orthopaedic surgeon, a surgeon who specialises in surgery that involves bones, muscles and joints or a podiatric surgeon, a podiatrist who specialises in foot surgery. Surgery is sometimes recommended for professional athletes and other sportspeople whose heel pain is adversely affecting their career. Plantar release surgery is the most widely used type of surgery for heel pain. The surgeon will cut the fascia to release it from your heel bone and reduce the tension in your plantar fascia. This should reduce any inflammation and relieve your painful symptoms. Surgery can be performed either as open surgery, where the section of the plantar fascia is released by making a cut into your heel or endoscopic or minimal incision surgery - where a smaller incision is made and special instruments are inserted through the incision to gain access to the plantar fascia. Endoscopic or minimal incision surgery has a quicker recovery time, so you will be able to walk normally much sooner (almost immediately), compared with two to three weeks for open surgery. A disadvantage of endoscopic surgery is that it requires both a specially trained surgical team and specialised equipment, so you may have to wait longer for treatment than if you were to choose open surgery. Endoscopic surgery also carries a higher risk of damaging nearby nerves, which could result in symptoms such as numbness, tingling or some loss of movement in your foot. As with all surgery, plantar release carries the risk of causing complications such as infection, nerve damage and a worsening of your symptoms after surgery (although this is rare). You should discuss the advantages and disadvantages of both techniques with your surgical team.
heel bursitis
Prevention

Heel pain is commonly caused from shoes that do not fit properly. In addition, shoes need to have ample cushioning and support, particularly through the heel, ball of the foot, and arch. Shoes should also be replaced if they become too worn. One sure sign of wear and tear is overly worn areas of a shoe's insoles. If the heel or ball of the foot is particularly worn, damage could easily occur since the bottom of the foot is not getting the cushioning it needs.
Leg Length Discrepancy Surgery For Adults
Overview
Have you noticed that your pants always fit a little weird or that you are always leaning to one leg when standing for awhile? If so, one of your legs may be longer than the other. This is known as a leg length discrepancy. There are two main reasons for a leg length discrepancy. One reason is that one of your leg bones (tibia or femur) is longer on one side. This is referred to as a true leg length discrepancy because the actual length of your bones is different. A second reason is that your pelvic bone may be rotated on one side making it appear that one leg is longer than the other. This is referred to as an apparent leg length discrepancy because the actual length of your leg bones is not different. In order to figure out if you have a true or apparent leg length discrepancy, your doctor may take an x-ray to measure the length of your leg bones or a simple measurement from your belly button to your ankle can help determine the reason. Over time, the leg length difference can cause stress on your low back, hips and knees, which may cause pain or discomfort.
Causes
Sometimes the cause of LLD is unknown, yet the pattern or combination of conditions is consistent with a certain abnormality. Examples include underdevelopment of the inner or outer side of the leg (hemimelias) or (partial) inhibition of growth of one side of the body of unknown cause (hemihypertrophy). These conditions are present at birth, but the limb length difference may be too small to be detected. As the child grows, the LLD increases and becomes more noticeable. In hemimelia, one of the two bones between the knee and the ankle (tibia or fibula) is abnormally short. There also may be associated foot or knee abnormalities. Hemihypertrophy or hemiatrophy are rare conditions in which there is a difference in length of both the arm and leg on only one side of the body. There may also be a difference between the two sides of the face. Sometimes no cause can be found. This type of limb length is called idiopathic. While there is a cause, it cannot be determined using currect diagnostic methods.
Symptoms
Often there are few or no symptoms prior to the age of 25-35. The most common symptom is chronic lower back pain, but also is frequently middle and upper back pain. Same-sided and repeated injury or pain to the hip, knee and/or ankle is also a hallmark of a long-standing untreated LLD. It is not uncommon to have buttock or radiating hip pain that is non-dermatomal (not from a disc) and tends to go away when lying down.
Diagnosis
Limb length discrepancy can be measured by a physician during a physical examination and through X-rays. Usually, the physician measures the level of the hips when the child is standing barefoot. A series of measured wooden blocks may be placed under the short leg until the hips are level. If the physician believes a more precise measurement is needed, he or she may use X-rays. In growing children, a physician may repeat the physical examination and X-rays every six months to a year to see if the limb length discrepancy has increased or remained unchanged. A limb length discrepancy may be detected on a screening examination for curvature of the spine (scoliosis). But limb length discrepancy does not cause scoliosis.
Non Surgical Treatment
For minor limb length discrepancy in patients with no deformity, treatment may not be necessary. Because the risks may outweigh the benefits, surgical treatment to equalize leg lengths is usually not recommended if the difference is less than 1 inch. For these small differences, the physician may recommend a shoe lift. A lift fitted to the shoe can often improve walking and running, as well as relieve any back pain that may be caused by the limb length discrepancy. Shoe lifts are inexpensive and can be removed if they are not effective.

shoe lifts for height
Surgical Treatment
Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age.
Have you noticed that your pants always fit a little weird or that you are always leaning to one leg when standing for awhile? If so, one of your legs may be longer than the other. This is known as a leg length discrepancy. There are two main reasons for a leg length discrepancy. One reason is that one of your leg bones (tibia or femur) is longer on one side. This is referred to as a true leg length discrepancy because the actual length of your bones is different. A second reason is that your pelvic bone may be rotated on one side making it appear that one leg is longer than the other. This is referred to as an apparent leg length discrepancy because the actual length of your leg bones is not different. In order to figure out if you have a true or apparent leg length discrepancy, your doctor may take an x-ray to measure the length of your leg bones or a simple measurement from your belly button to your ankle can help determine the reason. Over time, the leg length difference can cause stress on your low back, hips and knees, which may cause pain or discomfort.

Causes
Sometimes the cause of LLD is unknown, yet the pattern or combination of conditions is consistent with a certain abnormality. Examples include underdevelopment of the inner or outer side of the leg (hemimelias) or (partial) inhibition of growth of one side of the body of unknown cause (hemihypertrophy). These conditions are present at birth, but the limb length difference may be too small to be detected. As the child grows, the LLD increases and becomes more noticeable. In hemimelia, one of the two bones between the knee and the ankle (tibia or fibula) is abnormally short. There also may be associated foot or knee abnormalities. Hemihypertrophy or hemiatrophy are rare conditions in which there is a difference in length of both the arm and leg on only one side of the body. There may also be a difference between the two sides of the face. Sometimes no cause can be found. This type of limb length is called idiopathic. While there is a cause, it cannot be determined using currect diagnostic methods.
Symptoms
Often there are few or no symptoms prior to the age of 25-35. The most common symptom is chronic lower back pain, but also is frequently middle and upper back pain. Same-sided and repeated injury or pain to the hip, knee and/or ankle is also a hallmark of a long-standing untreated LLD. It is not uncommon to have buttock or radiating hip pain that is non-dermatomal (not from a disc) and tends to go away when lying down.
Diagnosis
Limb length discrepancy can be measured by a physician during a physical examination and through X-rays. Usually, the physician measures the level of the hips when the child is standing barefoot. A series of measured wooden blocks may be placed under the short leg until the hips are level. If the physician believes a more precise measurement is needed, he or she may use X-rays. In growing children, a physician may repeat the physical examination and X-rays every six months to a year to see if the limb length discrepancy has increased or remained unchanged. A limb length discrepancy may be detected on a screening examination for curvature of the spine (scoliosis). But limb length discrepancy does not cause scoliosis.
Non Surgical Treatment
For minor limb length discrepancy in patients with no deformity, treatment may not be necessary. Because the risks may outweigh the benefits, surgical treatment to equalize leg lengths is usually not recommended if the difference is less than 1 inch. For these small differences, the physician may recommend a shoe lift. A lift fitted to the shoe can often improve walking and running, as well as relieve any back pain that may be caused by the limb length discrepancy. Shoe lifts are inexpensive and can be removed if they are not effective.

shoe lifts for height
Surgical Treatment
Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age.
Addressing Mortons Neuroma
Overview
 Morton's Neuroma is a common foot problem associated with pain, swelling and/or an inflammation of a nerve, usually at the ball-of-the-foot between the 3rd and 4th toes. Symptoms of this condition include sharp pain, burning, and even a lack of feeling in the affected area. Morton's Neuroma may also cause numbness, tingling, or cramping in the forefoot.
Morton's Neuroma is a common foot problem associated with pain, swelling and/or an inflammation of a nerve, usually at the ball-of-the-foot between the 3rd and 4th toes. Symptoms of this condition include sharp pain, burning, and even a lack of feeling in the affected area. Morton's Neuroma may also cause numbness, tingling, or cramping in the forefoot.
Causes
The exact cause is as yet unclear. However there are a number of theories. Some expert s believe problems with the design of the foot makes some people more prone to Morton?s neuroma. Having flat feet or a high arch for example encourages the foot to slide forwards which can put excess pressure on the metatarsals. Bunions and hammer toes also increase the likelihood of developing Morton?s. However simply wearing high heels or any form of tight shoes that put pressure on the bones in the feet can also lead to a Morton?s . Typically the condition comes on between the age of 40 and 50. It is far more common in women than men - three out of four sufferers are women.
Symptoms
Neuroma pain is classically described as a burning pain in the forefoot. It can also be felt as an aching or shooting pain in the forefoot. Patients with this problem frequently say they feel like they want to take off their shoes and rub their foot. This pain may occur in the middle of a run or at the end of a long run. If your shoes are quite tight or the neuroma is very large, the pain may be present even when walking. Occasionally a sensation of numbness is felt in addition to the pain or even before the pain appears.
Diagnosis
The diagnosis of a Morton's neuroma can usually be made by the doctor when the history of pain suggests it and the examination elicits the symptoms. The foot is generally tender when the involved area is compressed and symptoms of pain and sometimes tingling can be elicited when the sides of the foot are squeezed. Magnetic resonance imaging (MRI) or ultrasound testing can be used to confirm the diagnosis if necessary.
Non Surgical Treatment
Treaments may include wearing wider shoes to reduce the squeezing force on the foot. Adding a specially made padding to shoes to offload the pressure on the ball of the foot (called a metatarsal dome) Addressing the foot and lower limb biomechanics. This involves looking at foot stability and if needed prescribing an orthotic device to correct your foot position. Anesthetic & Cortisone injections. This is done when the above treatments are insufficient. The trauma is sometimes so great that conservative treatment cannot control the inflammation or cause of the pain. A series of injections are performed to control the inflammation or to temporarily settle the nerve. An ultrasound and cortisone injection can be prescribed by your podiatrist.
Surgical Treatment
Interdigital neurectomy (removal of the diseased nerve) in right hands, should give satisfactory results almost all the time. Some of the reasons behind failure is when not enough nerve is dissected, mistakes in initial diagnosis, or bad handling of adjacent nerves, tendons and joint capsules during the operation. It is very common and acceptable to have some numbness in the area where the nerve used to be. This never causes any discomfort and often gets better in few years. It is crucial to address the biomechanical pathologies underlying the impingement of the nerve during and after the surgery.
 Morton's Neuroma is a common foot problem associated with pain, swelling and/or an inflammation of a nerve, usually at the ball-of-the-foot between the 3rd and 4th toes. Symptoms of this condition include sharp pain, burning, and even a lack of feeling in the affected area. Morton's Neuroma may also cause numbness, tingling, or cramping in the forefoot.
Morton's Neuroma is a common foot problem associated with pain, swelling and/or an inflammation of a nerve, usually at the ball-of-the-foot between the 3rd and 4th toes. Symptoms of this condition include sharp pain, burning, and even a lack of feeling in the affected area. Morton's Neuroma may also cause numbness, tingling, or cramping in the forefoot.Causes
The exact cause is as yet unclear. However there are a number of theories. Some expert s believe problems with the design of the foot makes some people more prone to Morton?s neuroma. Having flat feet or a high arch for example encourages the foot to slide forwards which can put excess pressure on the metatarsals. Bunions and hammer toes also increase the likelihood of developing Morton?s. However simply wearing high heels or any form of tight shoes that put pressure on the bones in the feet can also lead to a Morton?s . Typically the condition comes on between the age of 40 and 50. It is far more common in women than men - three out of four sufferers are women.
Symptoms
Neuroma pain is classically described as a burning pain in the forefoot. It can also be felt as an aching or shooting pain in the forefoot. Patients with this problem frequently say they feel like they want to take off their shoes and rub their foot. This pain may occur in the middle of a run or at the end of a long run. If your shoes are quite tight or the neuroma is very large, the pain may be present even when walking. Occasionally a sensation of numbness is felt in addition to the pain or even before the pain appears.
Diagnosis
The diagnosis of a Morton's neuroma can usually be made by the doctor when the history of pain suggests it and the examination elicits the symptoms. The foot is generally tender when the involved area is compressed and symptoms of pain and sometimes tingling can be elicited when the sides of the foot are squeezed. Magnetic resonance imaging (MRI) or ultrasound testing can be used to confirm the diagnosis if necessary.
Non Surgical Treatment
Treaments may include wearing wider shoes to reduce the squeezing force on the foot. Adding a specially made padding to shoes to offload the pressure on the ball of the foot (called a metatarsal dome) Addressing the foot and lower limb biomechanics. This involves looking at foot stability and if needed prescribing an orthotic device to correct your foot position. Anesthetic & Cortisone injections. This is done when the above treatments are insufficient. The trauma is sometimes so great that conservative treatment cannot control the inflammation or cause of the pain. A series of injections are performed to control the inflammation or to temporarily settle the nerve. An ultrasound and cortisone injection can be prescribed by your podiatrist.

Surgical Treatment
Interdigital neurectomy (removal of the diseased nerve) in right hands, should give satisfactory results almost all the time. Some of the reasons behind failure is when not enough nerve is dissected, mistakes in initial diagnosis, or bad handling of adjacent nerves, tendons and joint capsules during the operation. It is very common and acceptable to have some numbness in the area where the nerve used to be. This never causes any discomfort and often gets better in few years. It is crucial to address the biomechanical pathologies underlying the impingement of the nerve during and after the surgery.
Leg Length Discrepancy And Shoe Lifts
There are two different types of leg length discrepancies, congenital and acquired. Congenital means that you are born with it. One leg is structurally shorter compared to the other. Through developmental phases of aging, the human brain senses the step pattern and recognizes some variance. The human body typically adapts by dipping one shoulder to the "short" side. A difference of under a quarter inch is not very excessive, demand Shoe Lifts to compensate and typically does not have a serious effect over a lifetime.

Leg length inequality goes largely undiagnosed on a daily basis, yet this problem is very easily fixed, and can eradicate many instances of back discomfort.
Therapy for leg length inequality usually consists of Shoe Lifts. These are typically low cost, in most cases priced at under twenty dollars, compared to a custom orthotic of $200 or higher. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Back ache is the most widespread health problem impacting men and women today. Over 80 million men and women are afflicted by back pain at some stage in their life. It is a problem which costs companies millions of dollars every year because of time lost and production. Innovative and superior treatment methods are constantly sought after in the hope of decreasing the economical impact this issue causes.

Men and women from all corners of the world suffer the pain of foot ache as a result of leg length discrepancy. In a lot of these situations Shoe Lifts might be of very beneficial. The lifts are capable of easing any discomfort and pain in the feet. Shoe Lifts are recommended by many skilled orthopaedic practitioners".
So that they can support the body in a balanced manner, your feet have a vital role to play. Despite that, it's often the most overlooked area in the body. Some people have flat-feet which means there may be unequal force placed on the feet. This causes other parts of the body such as knees, ankles and backs to be affected too. Shoe Lifts guarantee that ideal posture and balance are restored.

Leg length inequality goes largely undiagnosed on a daily basis, yet this problem is very easily fixed, and can eradicate many instances of back discomfort.
Therapy for leg length inequality usually consists of Shoe Lifts. These are typically low cost, in most cases priced at under twenty dollars, compared to a custom orthotic of $200 or higher. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Back ache is the most widespread health problem impacting men and women today. Over 80 million men and women are afflicted by back pain at some stage in their life. It is a problem which costs companies millions of dollars every year because of time lost and production. Innovative and superior treatment methods are constantly sought after in the hope of decreasing the economical impact this issue causes.

Men and women from all corners of the world suffer the pain of foot ache as a result of leg length discrepancy. In a lot of these situations Shoe Lifts might be of very beneficial. The lifts are capable of easing any discomfort and pain in the feet. Shoe Lifts are recommended by many skilled orthopaedic practitioners".
So that they can support the body in a balanced manner, your feet have a vital role to play. Despite that, it's often the most overlooked area in the body. Some people have flat-feet which means there may be unequal force placed on the feet. This causes other parts of the body such as knees, ankles and backs to be affected too. Shoe Lifts guarantee that ideal posture and balance are restored.
Proven Methods To Diagnose Inferior Calcaneal Spur

Overview
A calcaneal spur (or heel spur) is a small osteophyte (bone spur) located on the calcaneus (heel bone). Calcaneal spurs are typically detected by a radiological examination (X-ray). When a foot bone is exposed to constant stress, calcium deposits build up on the bottom of the heel bone. Generally, this has no effect on a person's daily life. However, repeated damage can cause these deposits to pile up on each other,causing a spur-shaped deformity, called a calcaneal (or heel) spur. Obese people, flatfooted people, and women who constantly wear high-heeled shoes are most susceptible to heel spurs. An inferior calcaneal spur is located on the inferior aspect of the calcaneus and is typically a response to plantar fasciitis over a period, but may also be associated with ankylosing spondylitis (typically in children). A posterior calcaneal spur develops on the back of the heel at the insertion of the Achilles tendon. An inferior calcaneal spur consists of a calcification of the calcaneus, which lies superior to the plantar fascia at the insertion of the plantar fascia. A posterior calcaneal spur is often large and palpable through the skin and may need to be removed as part of the treatment of insertional Achilles tendonitis. These are also generally visible to the naked eye.
Causes
Heel spurs can form as a result of repeated strain placed on foot muscles and ligaments as well as from abnormally stretching the band of tissue connecting the heel and ball of the foot. Repeated injury to the membrane that lines the heel bone can also cause problems as can repeated tight pressure on the back of the heel. The causes can range from excessive walking (especially if unaccustomed to walking), running or jumping to improperly fitted or worn-out shoes. Runners, volleyball players, and tennis players, people who do step aerobics or stair climbing for exercise, those with flat feet, pregnant women, the obese and diabetics and those who wear tight-fitting shoes with a high heel are all prone to developing spurs (and plantar fasciitis) more readily.
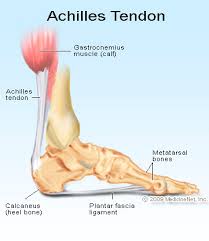
Symptoms
Heel spurs can be quite painful, but can just as likely occur with no symptoms at all. Plantar fasciitis is a contributing condition to heel spurs. The cause of the pain is not the heel spur itself but the soft-tissue injury associated with it. The feeling has been described as a knife or pin sticking into the bottom of your feet when you first stand up after sitting or laying down for a long period of time - a pain that later turns into a dull ache.
Diagnosis
A heel spur is often seen on X-ray as a bony protrusion, which can vary in size. However, because a Heel Spur only indicates increased load on the plantar fascia, and not pain, an ultra sound may be required to assess other actual cause of the heel pain such and may include checking to see if the plantar fascia is inflamed or degenerated.
Non Surgical Treatment
Treatment of heel spurs is the same as treatment of plantar fasciitis. Because these problems are related, the treatment is the same. The first step in the treatment of a heel spur is short-term rest and inflammation control. Here are the steps patients should take in order to cure the symptoms of plantar fasciitis and heel spurs. Avoiding the activity that caused the symptoms is the first step in treatment. For example, take a few day off jogging or prolonged standing/walking. Just resting usually helps to eliminate the most severe pain, and will allow the inflammation to begin to cool down. Icing will help to diminish some of the symptoms and control the heel pain. Icing is especially helpful after a sudden flare up of symptoms. Exercises and stretches are designed to relax the tissues that surround the heel bone. Some simple exercises, performed in the morning and evening, often help patients feel better quickly. Many patients will work with a physical therapist, or you can try some simple activities on your own. If you need some help, meet with a therapist for a few sessions to learn a program you can continue on your own.
Surgical Treatment
Almost 90% of the people suffering from heel spur get better with nonsurgical treatments. However, if the conservative treatments do not help you and you still have pain even after 9 to 12 months, your doctor may advise surgery for treating heel spur. The surgery helps in reducing the pain and improving your mobility. Some of the surgical techniques used by doctors are release of the plantar fascia. Removal of a spur. Before the surgery, the doctor will go for some pre-surgical tests and exams. After the operation, you will need to follow some specific recommendations which may include elevation of the foot, waiting time only after which you can put weight on the foot etc.
Prevention
To prevent this condition, wearing shoes with proper arches and support is very important. Proper stretching is always a necessity, especially when there is an increase in activities or a change in running technique. It is not recommended to attempt working through the pain, as this can change a mild case of heel spurs and plantar fascitis into a long lasting and painful episode of this condition.
What Are The Warning Signs Of Heel Spur
Overview
A heel spur is a buildup of calcium or a bone hook on the heel bone. This is typically the source of most heel pain. It usually takes an X-ray to see the heel spur protruding from the heel. Without proper heel spur treatment, a heel spur cause inflammation and lead to other ailments like plantar fasciitis and Achilles tendonitis. It is important to be examined by an orthopedic specialist.
Causes
The pain caused by heel spurs can be a sharp, stabbing pain when using the foot after a long period of rest. Sometimes it then reduces to a dull throb that can worsen when engaging in activities like jogging or jumping. People sometimes describe the pain of heel spurs and plantar fasciitis as a pin sticking into the bottom of the foot when they first stand up in the morning, this pain later turns into a bearable ache. The cause of the pain is generally not the heel spur itself, but the soft-tissue buildup associated with it. People often complain that the sharp pain returns after they stand up following sitting for a prolonged period of time.

Symptoms
Major symptoms consist of pain in the region surrounding the spur, which typically increases in intensity after prolonged periods of rest. Patients may report heel pain to be more severe when waking up in the morning. Patients may not be able to bear weight on the afflicted heel comfortably. Running, walking, or lifting heavy weight may exacerbate the issue.
Diagnosis
Diagnosis is made using a few different technologies. X-rays are often used first to ensure there is no fracture or tumor in the region. Then ultrasound is used to check the fascia itself to make sure there is no tear and check the level of scar tissue and damage. Neurosensory testing, a non-painful nerve test, can be used to make sure there is not a local nerve problem if the pain is thought to be nerve related. It is important to remember that one can have a very large heel spur and no plantar fasciitis issues or pain at all, or one can have a great deal of pain and virtually no spur at all.
Non Surgical Treatment
The most important part of treatment is to rest. Do not undertake activities which hurt the foot or aggravate symptoms as will only cause painful symptoms to persist. Apply an ice pack regularly for 10 minutes at a time every hour initially to reduce pain and inflammation of the surrounding tissues. As symptoms subside frequency of application can reduce to 2 or 3 times per day. Exercises and stretches to keep the foot and ankle strong and mobile are important as long as pain allows. Stretching the plantar fascia is important, especially if symptoms are worse in the morning. A plantar fasciitis night splint is excellent for stretching and preventing the plantar fascia tightening up over night. Anti-Inflammatory medicine (e.g. ibuprofen) may be prescribed by a doctor but always check with a medical professional first as taking some medications such as ibuprofen should not be done if the patient has asthma. Shoe inserts can help to take the pressure off of the spur and reduce pain. If these treatments do not significantly ease the symptoms then surgery may be an option.
Surgical Treatment
Almost 90% of the people suffering from heel spur get better with nonsurgical treatments. However, if the conservative treatments do not help you and you still have pain even after 9 to 12 months, your doctor may advise surgery for treating heel spur. The surgery helps in reducing the pain and improving your mobility. Some of the surgical techniques used by doctors are release of the plantar fascia. Removal of a spur. Before the surgery, the doctor will go for some pre-surgical tests and exams. After the operation, you will need to follow some specific recommendations which may include elevation of the foot, waiting time only after which you can put weight on the foot etc.
Prevention
To prevent this condition, wearing properly fitted shoes with good arch support is very important. If a person is overweight, weight loss can help diminish stress on the feet and help prevent foot problems. For those who exercise frequently and intensely, proper stretching is always necessary, especially when there is an increase in activities or a change in running technique. It is not recommended to attempt to work through the pain, as this can change a mild case of heel spurs and plantar fascitis into a long-lasting and painful episode of the condition.